Home Exercise Guide
Equipment That Works for GLP-1 Patients
Resistance training is non-negotiable on GLP-1 therapy. These are clinician-reviewed equipment choices suited to patients at all fitness levels — from low-impact cardio to progressive strength work.
GlantHealth Metabolic Medicine does not partner with, endorse, or receive compensation from any of the companies listed below. Products are suggested solely on the basis of clinical suitability for patients on GLP-1 therapy. Always consult your clinician before starting a new exercise programme.
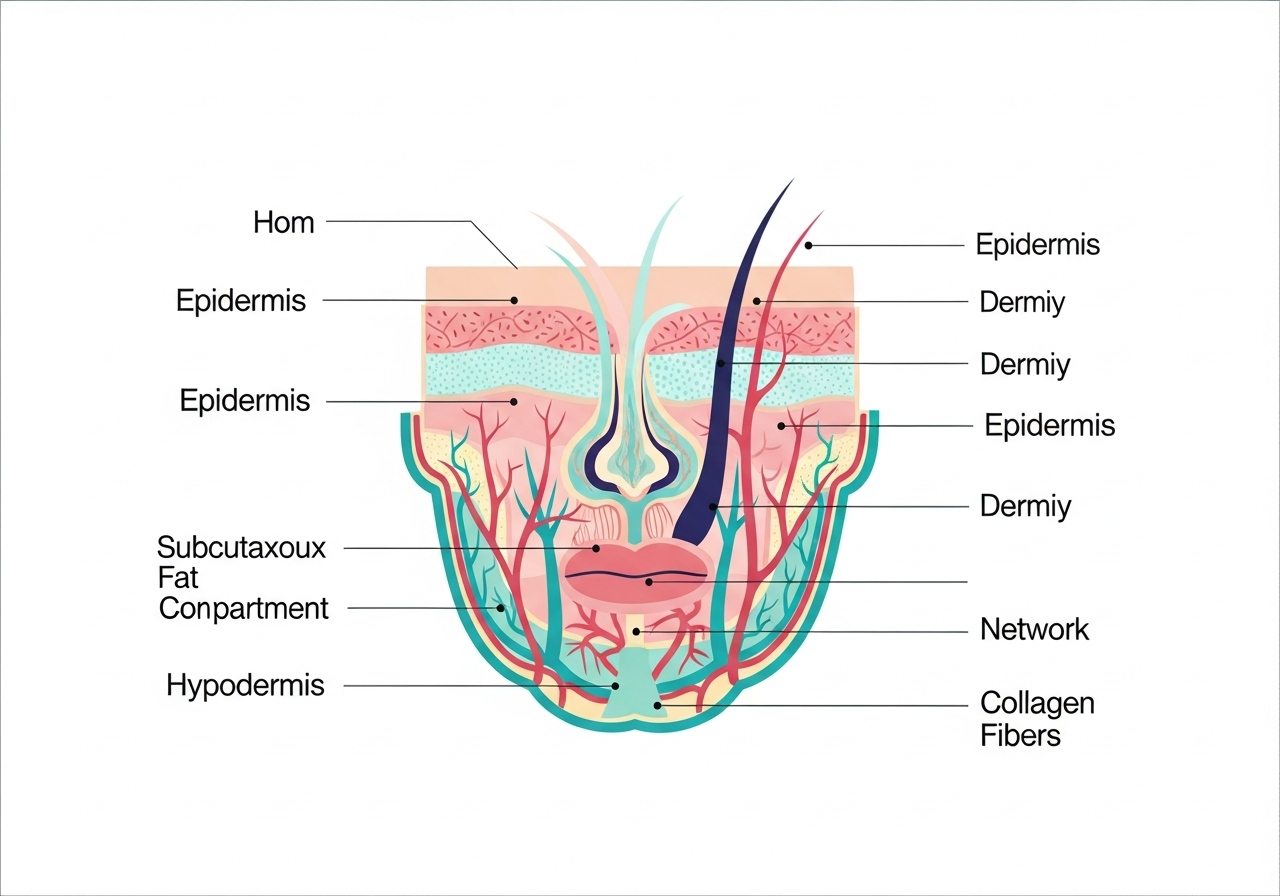
~25–40% of GLP-1 weight loss is lean mass
Without resistance training, you lose muscle — not just fat
Resistance training is the only proven fix
Walking and light cardio do not preserve lean mass in clinical trials
Home equipment removes the gym barrier
Consistency matters more than intensity — make it frictionless

Life Fitness Symbio Recumbent Cycle
Step-through design makes mounting easy at higher BMI. Dual-action arm handles add upper-body engagement. Multiple resistance levels for progressive overload.
Spirit Fitness CR1000ENT Recumbent Bike
Commercial-grade durability in a home footprint. Large seat, back support, and easy entry — well-suited for patients with limited mobility or recovering from deconditioning.
Matrix Total Body Cycle
Combines arm and leg cycling to maximise caloric output and engage more muscle groups simultaneously. Useful for patients who cannot weight-bear for long periods.
Martoni Cardio Speeder
Compact seated cardio unit with variable resistance. Good entry-level option for patients beginning exercise or working within nausea limitations post-injection.
Precor Breakaway™ Treadmill (Slat-Belt)
Slat-belt design distributes impact more evenly than traditional belts — significantly easier on knees, hips, and ankles. More natural running gait. Suitable for higher-weight users.
Matrix ClimbMill — Touch XL Console
Stair climber format with continuous rotating steps. Exceptional for glute, quad, and hamstring activation — directly targets muscles prone to atrophy on GLP-1 therapy. Touch XL console tracks workout metrics.

Precor Glutebuilder Selectorized Pendulum Kickback
Targets the gluteus maximus and hamstrings — muscle groups heavily affected by GLP-1–associated lean mass loss. Selectorized weight stack allows precise, safe progression. Pendulum motion reduces joint stress compared to cable kickbacks.

Resistance Vest
Adds distributed load (typically 5–25 kg) to any bodyweight movement — squats, lunges, stair-climbing, walking. Inexpensive, space-efficient, and progressive. GLP-1 clinical guidance specifically recommends progressive resistance — a vest is the most accessible way to achieve this at home.

Resistance Bands
Light, medium, and heavy colour-coded bands for progressive resistance. Covers rows, curls, presses, and leg work in a single inexpensive, portable kit. Ideal for GLP-1 patients at any fitness level — gentle enough to start with, strong enough to keep challenging muscles as strength returns.

Dumbbells (Light Fixed-Weight Set)
Start with 2–5 kg for upper body work — bicep curls, shoulder press, and lateral raises that target the arm and shoulder muscles most prone to atrophy on GLP-1 therapy. Fixed-weight dumbbells are safer and simpler than adjustable sets for beginners, with no plates to load or pins to set.

BOSU NexGen™ Pro Balance Trainer
Unstable surface training improves proprioception, ankle stability, and core engagement. Dual-sided use (dome up or flat side up) varies difficulty. Especially useful as rapid weight loss alters balance and gait.
Freemotion Pilates Reformer MS-01S
Spring-resistance reformer for full pilates, yoga, and Lagree-style workouts at home. Delivers resistance-based movement in a low-impact, joint-friendly format. Supports the deep postural muscles that protect the spine during rapid body recomposition.

InBody Dial H30
The InBody H30 is the home-use counterpart to the clinical InBody devices used in our clinic. Uses the same bioelectrical impedance analysis (BIA) technology to provide segmental body composition data — skeletal muscle mass, body fat percentage, and total body water — directly on your smartphone via the InBody app.
Home Exercise Guide · Workout Blueprint
Resistance Bands + Dumbbells + Incline Walking
A deceptively simple combination that covers all three pillars of GLP-1 exercise: muscle preservation, cardiovascular base, and joint-friendly movement. Here is why it works — and how to structure it.
Muscle preservation — the non-negotiable priority
Studies show 25–40% of GLP-1 weight loss can be lean mass without strength work. Bands and dumbbells apply progressive resistance to your muscles while the medication reduces your appetite — keeping your metabolism protected as the scale moves.
Incline walking + bands = loaded cardio without joint stress
Incline treadmill walking already activates glutes and hamstrings significantly more than flat walking. Add a resistance band above your knees and you recruit the glute medius — improving hip stability and burning more calories without high-impact loading. Ideal when GLP-1 fatigue makes intense cardio unrealistic.
Adapts instantly to how you feel on any given day
Bands and dumbbells let you scale resistance in seconds — no plates to load, no machines to adjust. On nausea days, drop the weight. On good days, increase it. Steady-state incline walking is also consistently better tolerated than HIIT when GI symptoms are present.
- Treadmill at 1–2% incline, easy conversational pace
- Mini band above knees: 10 lateral steps each direction
Goblet Squat Dumbbell + band above knees · 12 reps
Band cues knees to drive outward — protects form when GLP-1 fatigue affects coordination
Banded Romanian Deadlift Light dumbbells + band around feet · 10 reps
Targets hamstrings and glutes — critical for metabolic health and posture during weight loss
Resistance Band Row Band anchored, dumbbell in other hand · 12 reps/side
Counteracts the postural changes that accompany rapid weight loss
Incline Treadmill Walk 5 min · 5–8% incline · 2.5–3.0 mph · band above knees
You will feel this in your glutes. Hold the rails lightly if GLP-1 causes dizziness — no shame in that
- Flat treadmill walk at easy pace
- Banded glute bridges on floor: 15 reps
Exercise 1–2 hours after your largest meal of the day. Keep sessions to 30–45 minutes maximum in the first weeks — a short session you complete beats a long one you abandon.
Avoid floor-lying exercises on high-nausea days. Standing band work and incline walking are consistently better tolerated than floor-based abdominal exercises or anything that shifts your centre of gravity repeatedly.
GLP-1 medications reduce thirst cues alongside appetite. Sip electrolytes before incline work — you sweat more than you realise you are thirsty for.
Aim for 30–60 g protein within two hours of finishing. During rapid weight loss, post-workout nutrition is your primary lever for protecting lean mass — do not skip it.
Best starting position. Strongest glute activation with the least change to your natural gait. Start here.
Significantly harder. Requires shorter steps and a lighter band. Progress to this once above-knee feels easy.
Activates calves and shins. Useful if you experience foot tingling or numbness — a reported sensation in some GLP-1 users.
Muscle is your metabolic insurance policy. The medication is a tool — exercise is what makes the results last.
Not sure where to start? Our clinical team can help you build a realistic home exercise plan matched to your current fitness level, nausea pattern, and GLP-1 titration schedule. Message us on WhatsApp →